Click HERE To Buy Antabuse Online ↓
 Antabuse Vs Naltrexone: Which Suits You?
Antabuse Vs Naltrexone: Which Suits You?
How Antabuse and Naltrexone Work Differently
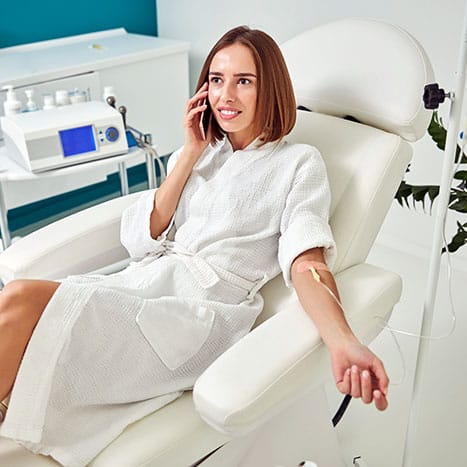
A patient sits with a clinician, weighing two paths: Antabuse creates an immediate, deterrent reaction if alcohol is consumed, while naltrexone targets brain receptors to blunt reward and reduce cravings over time. Both approaches aim to support recovery.
Antabuse blocks aldehyde dehydrogenase, causing unpleasant symptoms through acetaldehyde buildup; naltrexone is an opioid antagonist that inhibits mu receptors, diminishing alcohol’s pleasurable effects and lowering the drive to drink, clinically measurable over weeks respectively.
Onset differs: Antabuse produces immediate behavioral punishment when alcohol is present, while naltrexone’s benefit accrues with dosing and may require days to reach steady receptor blockade. Practical implications affect adherence and influence relapse risk.
Choosing depends on goals, medical history, liver function, comorbid opioid use, and willingness to tolerate deterrent reactions; shared decision-making with monitoring ensures the biological action aligns with personal recovery plans and supports long-term success.
| Antabuse | Naltrexone |
|---|---|
| Enzyme inhibition → aversive reaction | Opioid receptor blockade → reduced reward |
Comparing Effectiveness: Clinical Trials and Real World

Randomized trials give outcome measures, such as abstinence rates, relapse timing, and craving scores, allowing direct comparisons between medications. These controlled settings favor adherence and isolate pharmacologic effects, but they don’t always mirror everyday recovery
In clinics and community samples, effectiveness depends on adherence, co-occurring disorders, and support. antabuse's deterrent effect hinges on consistent dosing and patient motivation, while naltrexone shows broader craving reduction but requires engagement with treatment services.
Systematic reviews sometimes indicate modest superiority of one drug on select outcomes, yet observational cohorts reveal that side effects, limited access, and social instability frequently drive discontinuation and blunt real-world benefits across diverse patient populations.
Choosing between options requires personalized assessment: medical history, drinking patterns, psychiatric comorbidity, and readiness for change. Combining medication with counseling, family support, and practical monitoring yields the best translation of trial efficacy into lasting recovery.
Side Effects, Risks, and Safety Considerations
Choosing between medications often hinges on tolerability. Antabuse provokes an immediate, aversive reaction if alcohol is ingested—flushing, headache, nausea, even cardiovascular stress—which makes strict abstinence essential. Naltrexone’s common complaints are nausea, fatigue, and dizziness; more rarely it can elevate liver enzymes, so baseline liver tests are recommended.
Serious risks differ: antabuse can cause prolonged disulfiram-alcohol reactions and should never be used by someone who may inadvertently drink; it also interacts with certain medications. Naltrexone blocks opioid receptors, so it’s dangerous for patients using prescription or illicit opioids—precipitating withdrawal—and requires opioid-free status before initiation.
Shared safety practices include careful screening, informed consent, and regular follow-up. Monitor liver function, check for pregnancy, and review all substances including over-the-counter drugs. Discussing lifestyle, support systems, and emergency plans helps reduce harm and improves chances that whichever medication is chosen will be safe and effective.
Who Benefits Most: Patient Profiles and Contraindications

Imagine two paths to recovery: one suits people motivated by a behavioral deterrent, the other helps those needing craving reduction. antabuse appeals to individuals who can commit to strict abstinence and have strong social support; its effectiveness hinges on willingness to avoid alcohol entirely.
Naltrexone favors patients with heavy craving or binge patterns, including those who benefit from cue-triggered reductions in reward. It’s often chosen when relapse prevention and improved control are priorities.
Contraindications matter: Antabuse is unsafe in severe heart disease or uncontrolled diabetes and requires avoidance of any alcohol-containing products; naltrexone is contraindicated in acute hepatitis or opioid dependence. Shared decision-making with medical review and liver testing guides the safest, most effective choice.
Practical Issues: Dosing, Monitoring, Cost, Accessibility
Dosing often begins conservatively; antabuse commonly starts at 250 mg once daily, adjusted by a clinician. Clear written instructions and pill routines improve adherence.
Monitoring needs include liver tests, adherence checks, and quick reporting of reactions. Telehealth options and local clinics can ease follow up and reduce costs.
Accessibility varies by region; generics lower price but some clinics require supervised dispensing.
| Item | Typical | Notes |
|---|---|---|
| Cost | $10–150/month | Insurance affects out-of-pocket |
| Dosing | 250mg common initial dose | |
| Monitoring | Baseline and periodic | LFTs |
| Access | Widely available | generics pharmacies stock |
| Follow-up | Telehealth clinic | visits recommended |
Combining Medication with Therapy: Tips for Success
When Anna first started medication, she felt both relief and uncertainty; pairing her prescription with weekly counseling transformed those early gains into lasting change. Clinicians recommend integrating medication with cognitive behavioral therapy or motivational interviewing to address triggers, build coping skills, and reinforce adherence.
Start with clear goals: a shared plan between patient, prescriber, and therapist outlining expected benefits, duration, crisis strategies, and measures of progress. Regular communication among providers avoids conflicting advice and helps adjust medication dose, timing, or therapeutic focus when relapse signs appear.
Practical habits matter: schedule appointments, use pill organizers or supervised dosing if needed, and track cravings or moods in a journal to guide sessions. Stigma and ambivalence are common—normalizing setbacks and celebrating small victories keeps people engaged and improves outcomes. Peer support groups and family involvement often strengthen motivation and practical support as well.